Abstract
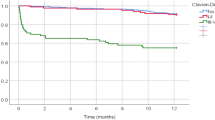
There are several predictor scales to assess the patients pre-operatively and thus inferring outcomes after surgery; for example, ASA (American Society of Anesthesiologists) scoring, SORT (Surgical Outcome Risk Tool), and APACHE II (Acute Physiology and Chronic Health Disease Classification System II). However, most surgeons would see advancing age as an important predictor of surgical outcome especially after a major surgery. Chronological age may not be the only determinant outcome after surgery. In a group of colonic cancer patients, we compared standard pre-defined outcomes in subjects above 80 years to below 80 years. Specifically we compared Clinical, surgical, pathological, and survival data of 71 oldest old patients (≥80 years) and 67 younger (<80 years) patients treated by surgery between January 2018 and January 2020. No differences in terms of intra- and peri-operatory mortality, post-operative complications, length of hospital stay, and needing of Intensive Care Unit were found between the two groups. Univariate and multivariate analyses identified, above all, laparotomy, anastomotic leak, lymph node, and hematogenous metastasis as independent prognostic factors for a worse outcome. The Kaplan-Meier curves demonstrated that both the 180-day survival and the overall survival overlapped. The results of our study highlight how chronological age should not to be considered a barrier for a proper treatment, pointing at surgery as a feasible approach also in elderly patients. Our findings may open the way for planning “ad hoc” screening protocols in this subset of patient.

Similar content being viewed by others
References
Itatani Y, Kawada K, Sakai Y (2018) Treatment of elderly patients with colorectal cancer. BioMed Res Int 2018:2176056. https://doi.org/10.1155/2018/2176056
Crews DE, Zavotka S (2006) Aging, disability, and frailty: implications for universal design. J Physiol Anthropol. 25:113–118
Korc-Grodzicki B, Holmes HM, Shahrokni A (2015) Geriatric assessment for oncologists. Cancer Biol Med 12(4):261–74. https://doi.org/10.7497/j.issn.2095-3941.2015.0082
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F (2021) Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71(3):209–249. https://doi.org/10.3322/caac.21660
Global Health Estimates 2020 (2020) Deaths by cause, age, sex, by country and by region, 2000-2019. World Health Organization, Geneva
Podda M, Sylla P, Baiocchi G et al (2021) Multidisciplinary management of elderly patients with rectal cancer: recommendations from the SICG (Italian Society of Geriatric Surgery), SIFIPAC (Italian Society of Surgical Pathophysiology), SICE (Italian Society of Endoscopic Surgery and new technologies), and the WSES (World Society of Emergency Surgery) International Consensus Project. World J Emerg Surg 16:35. https://doi.org/10.1186/s13017-021-00378-9
Keum N, Giovannucci E (2019) Global burden of colorectal cancer: emerging trends, risk factors and prevention strategies. Nat Rev Gastroenterol Hepatol 16(12):713–732. https://doi.org/10.1038/s41575-019-0189-8
Mukai T, Akiyoshi T, Ueno M, Fukunaga Y, Nagayama S, Fujimoto Y, Konishi T, Ikeda A, Yamaguchi T (2014) Outcomes of laparoscopic surgery for colorectal cancer in oldest-old patients. Surg Laparosc Endosc Percutan Tech. 24(4):366–9. https://doi.org/10.1097/SLE.0b013e31829012ca
Lund CM, Vistisen KK, Olsen AP, Bardal P, Schultz M, Dolin TG, Rønholt F, Johansen JS, Nielsen DL (2021) The effect of geriatric intervention in frail older patients receiving chemotherapy for colorectal cancer: a randomised trial (GERICO). Br J Cancer 124(12):1949–1958. https://doi.org/10.1038/s41416-021-01367-0
Podda M, Sylla P, Baiocchi G, Adamina M, Agnoletti V, Agresta F, Ansaloni L, Arezzo A, Avenia N, Biffl W, Biondi A, Bui S, Campanile FC, Carcoforo P, Commisso C, Crucitti A, De’Angelis N, De’Angelis GL, De Filippo M, De Simone B, Di Saverio S, Ercolani G, Fraga GP, Gabrielli F, Gaiani F, Guerrieri M, Guttadauro A, Kluger Y, Leppaniemi AK, Loffredo A, Meschi T, Moore EE, Ortenzi M, Pata F, Parini D, Pisanu A, Poggioli G, Polistena A, Puzziello A, Rondelli F, Sartelli M, Smart N, Sugrue ME, Tejedor P, Vacante M, Coccolini F, Davies J, Catena F (2021) Multidisciplinary management of elderly patients with rectal cancer: recommendations from the SICG (Italian Society of Geriatric Surgery), SIFIPAC (Italian Society of Surgical Pathophysiology), SICE (Italian Society of Endoscopic Surgery and new technologies), and the WSES (World Society of Emergency Surgery) International Consensus Project. World J Emerg Surg 16(1):35 https://doi.org/10.1186/s13017-021-00378-9.
Peltrini R, Imperatore N, Carannante F, Cuccurullo D, Capolupo GT, Bracale U, Caricato M, Corcione F (2021) Age and comorbidities do not affect short-term outcomes after laparoscopic rectal cancer resection in elderly patients. A multi-institutional cohort study in 287 patients. Updates Surg 73(2):527–537
Giardini V, Gianotti L (2020) Should radical surgery for rectal cancer be offered to elderly population? A propensity-matching analysis on short- and long-term outcomes. Updates Surg 72(3):801–809. https://doi.org/10.1007/s13304-020-00717-6
Jung YH, Kim JY, Jang YN, Yoo SH, Kim GH, Lee KM, Lee IK, Chung SM, Woo IS (2018) Clinical characteristics and treatment propensity in elderly patients aged over 80 years with colorectal cancer. Korean J Intern Med 33(6):1182–1193. https://doi.org/10.3904/kjim.2016.181
Ng O, Watts E, Bull CA, Morris R, Acheson A, Banerjea A (2016) Colorectal cancer outcomes in patients aged over 85 years. Ann R Coll Surg Engl 98(3):216–21. https://doi.org/10.1308/rcsann.2016.0085
Krzyzanowska MK, Regan MM, Powell M, Earle CC, Weeks JC (2009) Impact of patient age and comorbidity on surgeon versus oncologist preferences for adjuvant chemotherapy for stage III colon cancer. J Am Coll Surg. 208:202–209
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP; STROBE Initiative (2014) The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement: guidelines for reporting observational studies. Int J Surg 12(12):1495–1499 https://doi.org/10.1016/j.ijsu.2014.07.013
Pedrazzani C, Secci F, Fernandes E, Jelovskijs I, Turri G, Conti C, Ruzzenente A, Guglielmi A (2019) Early ileostomy reversal after minimally invasive surgery and ERAS program for mid and low rectal cancer. Updates Surg 71(3):485–492. https://doi.org/10.1007/s13304-018-0597-2
Tejedor P, González Ayora S, Ortega López M, León Arellano M, Guadalajara H, García-Olmo D, Pastor C (2021) Implementation barriers for Enhanced Recovery After Surgery (ERAS) in rectal cancer surgery: a comparative analysis of compliance with colon cancer surgeries. Updates Surg. https://doi.org/10.1007/s13304-021-01115-2
Planellas Giné P, Cornejo Fernández L, Salvador Rosés H, Buxó Pujolras M, Farrés Coll R, Hernandez Yague X, Canals Subirats E, Gil Garcia J, Rodríguez Hermosa JI, Codina Cazador A (2020) Delaying surgery by more than 10 weeks after long-course neoadjuvant radiotherapy in locally advanced rectal cancer patients improves pathologic complete response. Updates Surg 72(2):453-461https://doi.org/10.1007/s13304-020-00747-0
Benson AB, Venook AP, Al-Hawary MM, Arain MA, Chen YJ, Ciombor KK, Cohen S, Cooper HS, Deming D, Farkas L, Garrido-Laguna I, Grem JL, Gunn A, Hecht JR, Hoffe S, Hubbard J, Hunt S, Johung KL, Kirilcuk N, Krishnamurthi S, Messersmith WA, Meyerhardt J, Miller ED, Mulcahy MF, Nurkin S, Overman MJ, Parikh A, Patel H, Pedersen K, Saltz L, Schneider C, Shibata D, Skibber JM, Sofocleous CT, Stoffel EM, Stotsky-Himelfarb E, Willett CG, Gregory KM, Gurski LA (2021) Colon Cancer, Version 2.2021, NCCN Clinical Practice Guidelines in Oncology. J Natl Compr Canc Netw 19(3):329–359 https://doi.org/10.6004/jnccn.2021.0012
André T, Shiu KK, Kim TW, Jensen BV, Jensen LH, Punt C, Smith D, Garcia-Carbonero R, Benavides M, Gibbs P, de la Fouchardiere C, Rivera F, Elez E, Bendell J, Le DT, Yoshino T, Van Cutsem E, Yang P, Farooqui MZH, Marinello P, Diaz LA Jr; KEYNOTE-177 Investigators (2020) Pembrolizumab in Microsatellite-Instability-High Advanced Colorectal Cancer. N Engl J Med 383(23):2207–2218 https://doi.org/10.1056/NEJMoa2017699
Zhao M, Liu H, Tang Y, Meng X, Yu J, Wang Q, Zhou Q, Leng SX, Zhang H (2017) Clinicopathologic features and prognostic factors for patients with colorectal cancer who are 75 years and older. Oncotarget. 8(45):80002–80011. https://doi.org/10.18632/oncotarget.20656
Roque-Castellano C, Fariña-Castro R, Nogués-Ramia EM, Artiles-Armas M, Marchena-Gómez J (2020) Colorectal cancer surgery in selected nonagenarians is relatively safe and it is associated with a good long-term survival: an observational study. World J Surg Oncol 18(1):120. https://doi.org/10.1186/s12957-020-01895-8
Townsley C, Pond GR, Peloza B et al (2005) Analysis of treatment practices for elderly cancer patients in Ontario, Canada. J Clin Oncol 23:3802–3810
Surgery for colorectal cancer in elderly patients: a systematic review. Colorectal Cancer Collaborative Group. Lancet. 2000;356:968-974
Kunitake H, Zingmond DS, Ryoo J, Ko CY (2010) Caring for octogenarian and nonagenarian patients with colorectal cancer: what should our standards and expectations be? Dis Colon Rectum 53:735–743
Menegozzo CMA, Teixeira-Junior F, Dias do Couto-Netto S, Martins-Junior O, de Olivera Bernini C, Massazo Utiyama E (2019) Outcomes of elderly patients undergoing emergency surgery for complicated colorectal cancer: a retrospective cohort study. Clinics (Sao Paulo) 74:e1074
Santos AC, Martins LL, Brasil AM, Pinto SA, Neto SG, Oliversa EC (2014) emergency surgery for complicated colorectal cancer in central Brasil. J Coloproctol 34(2):104–8
Vignali A, Elmore U, Guarneri G, De Ruvo V, Parise P, Rosati R (2021) Enhanced recovery after surgery in colon and rectal surgery: identification of predictive variables of failure in a monocentric series including 733 patients. Updates Surg 73(1):111–121. https://doi.org/10.1007/s13304-020-00848-w
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Patient collection was performed by Dr. Marco Arganini, Dr. Bruno Perotti, and Dr. Geri Fratini. Data collection was performed by Dr. Luigi Spagnoli, Dr.ssa Federica Petrelli, Dr.ssa Elena Sabattini, and Dott.ssa Maura Rossi. Statistical analysis was exploited by Dr.ssa Alessia D’Ignazio. Data and results analysis were performed by Dr. Marco Arganini, Dr.ssa Maria Raffaella Ambrosio, and Dr. Andrea Cavazzana. The first draft of the manuscript was written by Dr. Bruno Perotti, Dr. Marco Arganini and Dr.ssa Maria Raffaella Ambrosio and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests. Authors are responsible for correctness of the statements provided in this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Perotti, B., D’Ignazio, A., Fratini, G. et al. Comparison of Survival Analysis After Surgery for Colorectal Cancer in Above 80 Years (Oldest-Old) and Below 80 Years Old Patients. Indian J Surg 85, 313–321 (2023). https://doi.org/10.1007/s12262-022-03417-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12262-022-03417-0